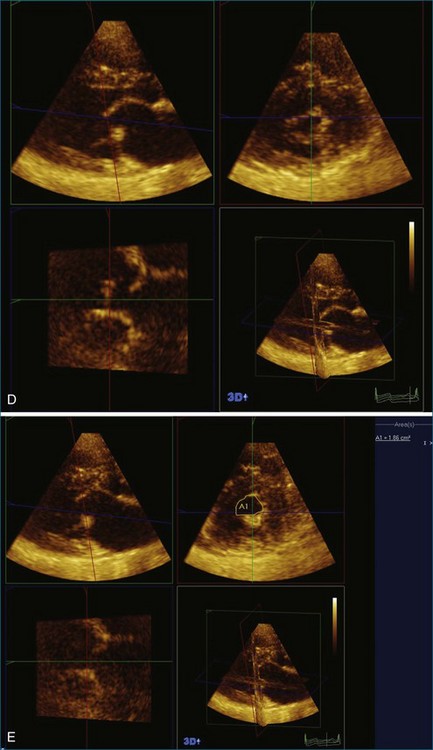
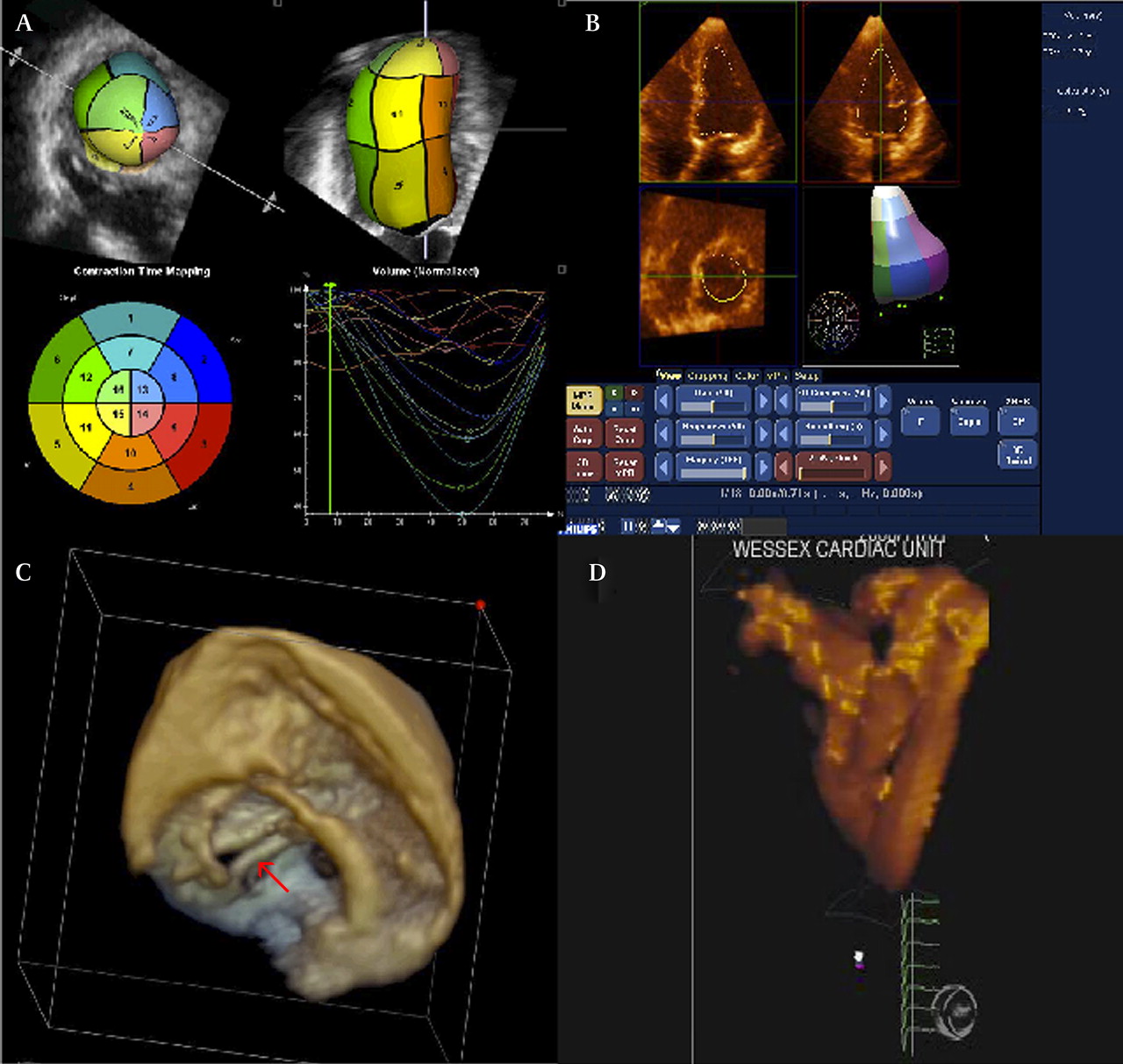
8-10 Several imaging modalities have been integrated into the clinical use for the evaluation of AAPs, including magnetic resonance imaging and computed tomography (CT), with transoesophageal echocardiogram (TEE) considered as the leading diagnostic tool due to its favourable availability and the lack of radiation and/or contrast media compared with the other modalities. 7 In addition to the plaque thickness, other morphologic features, such as ulcerations or mobile components, have been identified to increase the embolic risk. 1, 5, 6 Moreover, this cut-off has been associated with increased 1-year incidence of recurrent vascular events (transient ischaemic attacks and minor strokes). 2-4 A cut-off of 4 mm has been shown to be clinically relevant for risk stratification with one-third of the patients with cryptogenic stroke having large plaques (>4 mm in thickness) in the aortic arch. 1 Furthermore, AAPs are regarded as markers of the atherosclerotic burden of the vascular tree as in the coronary and peripheral arteries. The rate of irregular AAPs increased from 29 to 65% when assessed with 3D imaging compared with 2D imaging.Īortic atherosclerotic plaque, transoesophageal echocardiography, two-dimensional, three-dimensional IntroductionĪortic atherosclerotic plaques (AAPs), especially when located at the arch, are one of the major causes of spontaneous and iatrogenic stroke and peripheral emboli along with atrial fibrillation and carotid atherosclerosis. The rate of complex AAPs (defined by AAP thickness of ≥4 mm) was two-fold higher with 3D imaging than with 2D imaging (27% with 2D imaging alone vs. The AAP thickness estimation was significantly greater in the 3D mode than in the 2D mode (0.51 ± 0.33 vs. The AAP contour was defined qualitatively as regular or irregular in each mode. If focal intimal thickening (suggestive of AAP) was detected, the 3D zoom algorithm was exercised on the specific site with further post-processing on a Q-lab workstation to measure its thickness in the X, Y, and Z dimensions. The thoracic aorta was studied from arch to distal descending aorta, using the x-plane mode (simultaneous short- and long-axis views). The study included 67 patients (aged 70 ± 15 years, 35 men), who had routine TEE studies.

